How to enhance insurer agility in 2026

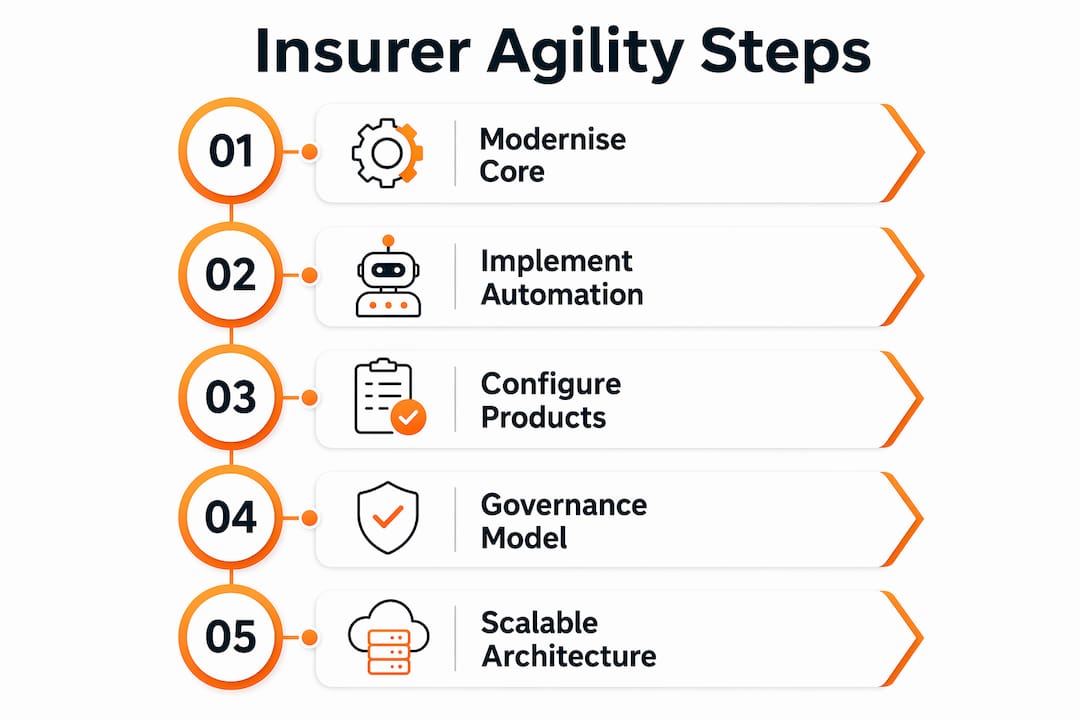
Insurer agility is defined as the capacity to adapt products, services, and operations quickly in response to market shifts, regulatory change, and customer demand. Enhancing it requires a deliberate combination of core system modernisation, targeted automation, and governance structures that give teams the freedom to move fast without creating compliance risk. For European P&C insurers, the stakes are high: legacy architectures slow product launches, inflate service costs, and leave organisations unable to respond when conditions change. The strategies covered here draw on the latest thinking from McKinsey, BCG, Duck Creek, and Ibapplications to give you a practical path forward.
How to enhance insurer agility through core system modernisation
The most direct route to operational flexibility is replacing or restructuring the core systems that govern policy administration, rating, and claims. Legacy monolithic platforms create coupling between business logic and infrastructure that makes even minor product changes expensive and slow. Structured build-versus-buy assessments reduce transformation risk and improve speed to change by forcing a disciplined comparison of vendor capability against internal build cost before any commitment is made.
The architecture that emerges from modernisation matters as much as the decision to modernise. Cloud-based, API-first platforms with microservices design allow individual components, such as rating engines or billing modules, to be updated independently without touching the rest of the system. Multi-jurisdictional compliance and scalable multi-line business become achievable when infrastructure is flexible and ecosystem connectivity is built in from the start. This is particularly relevant for European insurers operating across multiple regulatory regimes.
A phased roadmap that prioritises quick wins builds momentum and demonstrates return on investment before the full transformation is complete. The alternative, a big-bang replacement, concentrates risk and delays value. Governance frameworks that define clear ownership, decision rights, and success metrics keep phased programmes on track without creating bureaucratic drag.
- Conduct a structured build-versus-buy assessment before selecting vendors or committing to internal development.
- Adopt an API-first, microservices architecture to decouple components and enable independent release cycles.
- Define a phased roadmap with measurable milestones and governance checkpoints at each stage.
- Establish multi-jurisdiction compliance requirements as non-negotiable design constraints from day one.
| Modernisation approach | Agility impact |
|---|---|
| Monolithic core replacement | High risk, high reward; requires strong governance and phased execution |
| API-first modular upgrade | Lower risk; enables incremental improvement and faster release cycles |
| Cloud migration with existing architecture | Moderate gain; reduces infrastructure cost but does not address logic coupling |
| Greenfield cloud-native build | Maximum flexibility; best suited to new lines or subsidiaries |
Pro Tip: When evaluating vendors, ask specifically how they handle Evergreen updates. A platform that pushes mandatory upgrades without disrupting your configuration is worth a significant premium over one that requires manual migration with each release.
How can automation reduce service workloads and improve customer responsiveness?
Automation delivers the fastest measurable gains in improving insurance responsiveness because it targets the highest-volume, lowest-complexity interactions first. AI chatbots and voice bots handle policy queries, renewal reminders, and first notice of loss capture without adding headcount. The critical distinction is between bots that answer questions and bots that complete actions end-to-end. Only the latter produces genuine workload reduction; the former simply shifts the interaction from a human agent to a digital one.

Automated document collection via SMS and email workflows removes one of the most persistent sources of claims delay. When a claimant submits a loss notification, the system immediately requests supporting documents through the claimant’s preferred channel, validates completeness on receipt, and flags exceptions for human review. This eliminates the back-and-forth that typically adds days to a cycle time.
Proactive claims status communication is one of the highest-return automation investments available. Proactive multi-channel notifications cut inbound status calls by 60 to 75 per cent and shorten perceived cycle time by three to five days. Customers who receive regular, accurate updates do not call to ask where their claim stands. That frees your service team to handle genuinely complex interactions.
- Deploy AI chatbots for high-frequency queries: policy documents, payment confirmations, and renewal dates.
- Automate FNOL capture with structured data fields that prevent incomplete submissions from entering the workflow.
- Set up proactive SMS and email status updates triggered by claims milestones, not just agent action.
- Use multi-channel fallback logic so that if a customer does not open an email, an SMS follows automatically.
- Review notification cadence regularly to avoid over-communication that trains customers to ignore updates.
Pro Tip: Data completeness at FNOL intake is the single most important control in any automation programme. A missing field at intake creates a manual rework loop that can negate every efficiency gain downstream. Build validation rules into the intake form before you build anything else.
What role do configurable product tools play in boosting insurer agility?
Product launch speed is a direct measure of insurer agility. The time between identifying a market opportunity and having a compliant, rated product available for sale determines whether you capture that opportunity or watch a competitor take it. AI-native agentic product configurators address this directly. Duck Creek’s agentic product configurator reduces product implementation timelines by up to 50 per cent by unifying the workflow from requirements capture through to deployment in a single governed environment.
The governance dimension is what separates genuine agility from reckless speed. Human-in-the-loop validation ensures that AI-generated product configurations are reviewed and approved before they reach production. This maintains compliance and accuracy while still compressing the timeline significantly. The result is a product launch process that is both faster and more consistent than manual configuration.
Reuse of product variants across geographies and lines of business is where the compounding value appears. Once a product structure is built and validated in one market, adapting it for a second jurisdiction requires configuration changes rather than a full rebuild. For European insurers managing products across multiple regulatory environments, this capability is a material competitive advantage. You can read more about the steps involved in launching insurance products efficiently in a related guide from Ibapplications.
| Product launch approach | Time to market | Compliance control | Reusability |
|---|---|---|---|
| Manual configuration by IT teams | Slow (months) | High but inconsistent | Low |
| AI-assisted configurator with human review | Fast (weeks) | High and consistent | High |
| Fully automated without human review | Very fast | Risk of compliance gaps | Medium |
How does governance and architectural design support scalable agility?
Speed without governance creates technical debt and compliance exposure. The organisations that sustain agility at scale are those that have designed governance into their architecture rather than bolting it on afterwards. Federated operating models balance central standards with local execution speed by giving central teams responsibility for defining reusable components and funding priorities, while local teams retain the autonomy to adopt and adapt those components for their specific markets.
Microservices architecture reinforces this model at the technical level. When rating logic, policy administration, and claims processing run as independent services, each can be updated, tested, and deployed without affecting the others. Decoupling rating logic from monolithic systems reduces release cycles and audit friction simultaneously. Immutable, time-stamped audit trails built into each service provide the traceability that regulators require without slowing the release process.
Governance by alignment and reuse outperforms governance by control. The traditional model, where a central architecture board approves every change, creates bottlenecks that negate the speed gains from modernisation. The better model uses shared backlogs, centralised KPIs, and reusable component libraries to keep teams aligned without requiring approval at every step.
- Adopt a federated model where central teams own standards and local teams own execution.
- Build immutable audit trails into every service from the start, not as a retrofit.
- Replace approval-based governance with shared KPIs and reusable component libraries.
- Measure agility outcomes with scorecards that track release frequency, time to market, and defect rates alongside cost metrics.
“Governance for agile modernisation should emphasise collaboration, adaptability, and reuse to avoid duplicated effort and speed execution.” BCG, 2026
Modernising insurance operations for digital agility requires this architectural discipline as a foundation, not an afterthought.
Key takeaways
Insurer agility scales when core system modernisation, targeted automation, configurable product tooling, and federated governance are pursued together rather than in isolation.
| Point | Details |
|---|---|
| Modernise architecture first | API-first, microservices design unlocks independent release cycles and multi-jurisdiction flexibility. |
| Automate at the highest-volume touchpoints | FNOL capture and proactive status updates deliver the fastest measurable gains in responsiveness. |
| Use AI-assisted product configuration | Agentic configurators can cut product launch timelines by up to 50 per cent while maintaining compliance. |
| Govern by alignment, not control | Federated models with shared KPIs outperform centralised approval boards in sustained agility programmes. |
| Measure agility outcomes explicitly | Track release frequency, time to market, and defect rates to demonstrate and sustain transformation value. |
Where most agility programmes go wrong
The most common failure I see is treating agility as an IT project rather than a business and IT joint agenda. Transformation programmes that are owned exclusively by technology teams tend to optimise for architectural elegance rather than business outcomes. The insurers that move fastest are those where the chief operating officer and the chief information officer share a single set of success metrics and a joint accountability for delivery.
The second failure is the big-bang instinct. Executives under pressure to show results want a single, transformative programme that solves everything at once. In practice, phased modernisation with early quick wins builds the organisational capability and the political capital to sustain a multi-year programme. A chatbot that handles 40 per cent of inbound policy queries in month three is worth more to the programme than a perfect architecture that delivers nothing for eighteen months.
The third issue is data quality at the point of intake. I have seen automation programmes that looked impressive in design but collapsed in production because incomplete FNOL data created manual rework loops that consumed more resource than the original process. Completeness validation at intake is unglamorous work, but it is the foundation on which every downstream automation depends.
Finally, governance nuance matters enormously when scaling across multiple European markets. A model that works in one jurisdiction will not transfer automatically to another with different regulatory requirements and distribution structures. Federated reuse, where central components are adapted rather than replicated, is the only model that scales without creating a maintenance burden that eventually overwhelms the agility gains.
— Tuna
How IBSuite supports agile insurance operations
Ibapplications builds IBSuite as a cloud-native, API-first core insurance platform designed specifically for P&C insurers that need to move quickly without sacrificing compliance or control. IBSuite covers the full insurance value chain, from rating and underwriting through to claims, billing, and financial sub-ledger, within a single modular architecture that supports independent updates across components. Insurers using IBSuite can launch new products faster, adapt to regulatory changes without full system overhauls, and scale across multiple European markets from a shared platform foundation. If you are evaluating how a modern core platform could accelerate your agility programme, book a demo to see IBSuite in practice.
FAQ
What is insurer agility and why does it matter?
Insurer agility is the ability to adapt products, pricing, and operations quickly in response to market or regulatory change. It matters because slow adaptation leads to lost market share, higher operational costs, and compliance risk.
How long does core system modernisation typically take?
A phased modernisation programme typically delivers initial value within six to twelve months, with full transformation spanning two to four years depending on the complexity of existing systems and the number of product lines involved.
Can automation genuinely reduce claims service workload?
Yes. Proactive claims status communications alone cut inbound calls by 60 to 75 per cent, and end-to-end automation of FNOL capture removes the manual rework loops that inflate handling time.
What is a federated governance model in insurance modernisation?
A federated model gives central teams responsibility for defining standards and reusable components, while local teams retain autonomy to execute within those standards. BCG identifies this approach as the governance structure that best sustains agility at scale.
How do AI-powered product configurators improve compliance?
AI-powered configurators with human-in-the-loop validation generate product structures automatically but require human review before deployment. This maintains regulatory accuracy while compressing the configuration timeline significantly compared to fully manual processes.
Recommended
- Drivers of Digital Transformation in the Insurance Industry – Digital Insurance Platform | IBSuite Insurance Software | Modern Insurance System
- Embracing Compliance through Next-Generation Insurance Platforms – Digital Insurance Platform | IBSuite Insurance Software | Modern Insurance System
- 7 Key Insurtech Trends 2025 for P&C Insurance Leaders – Digital Insurance Platform | IBSuite Insurance Software | Modern Insurance System
- Insurance marketplace models 2026: 50% faster launches